The CPSM Approach

EMS agencies across the country are being stressed to the limit. Staffing shortages, skyrocketing expenses, rising response volumes – many for low-acuity responses – supply chain disruptions and economic models that only reimburse for ambulance transport are converging to cause failures for EMS systems in many communities.
CPSM’s EMS subject matter experts (SMEs) are rising to these challenges since many are actively working through these issues every day! Some are internationally recognized for their approach to rationale, data-driven, and patient-centered approaches to effective and efficient service delivery.
We start each project with a detailed analysis of EMS call data to provide a comprehensive review of emergency medical services including a detailed analysis of workloads and response times. The analysis of the workloads begins with an in-depth study of the types of calls handled and their severity. The goal is to identify the fundamental nature of the emergency medical challenge faced by the community and the EMS agency. We pay special attention to the most critical emergencies such as heart attack and serious vehicular accidents. We also look at the clinical, operational, financial, and patient experiential performance of the EMS agency, whether it’s fire-based, 3rd service governmental, hospital-based, or contracted.
For each EMS call type, we determine the time spent on-scene and the number of personnel who worked the scene. The data is aggregated to determine an overall average total time spent on EMS calls. We also determine how much EMS calls contribute to the workload of first response and transport resources. We illustrate any dramatic variations by time of day and day of week, as well as seasonal variations.
While data related to responses, response times and clinical performance are important, in today’s environment, they are not the only things to be considered for the delivery of EMS. Alternate delivery models such as community paramedicine, treat and non-transport programs, transport to alternate destinations, and resourceful economic models are solutions that CPSM’s SMEs have helped implement in many communities as mitigation factors to improve EMS delivery and effectiveness.
CPSM’s EMS SMEs have extensive experience with revenue cycle management for EMS delivery and can provide a detailed analysis of the revenue cycle to help assure maximization of revenue generation to potentially reduce the need for a public subsidy.
Cost Analytics Examples
Our operations team for EMS will go beyond simply looking at the TIME your service took to respond and drill down to determine cost analytics. Examples of those are:
Total Annual Cost
- Cost per Unit Hour
- Total costs ÷Produced or Scheduled Unit Hours
- Cost per Response
- Total costs ÷Responses
- Cost per Transport
- Total costs ÷Transports
- Cost per Capita
- Total costs ÷Population Served
- Fixed vs. Variable Cost Categorization
- Cost to manage the service | Stair step costs | Cost to call
Creating a Clinical Report Card
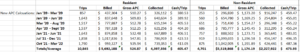
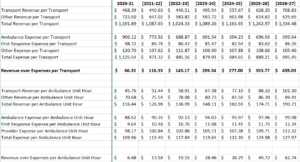
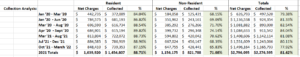

EMS is also about managing using key performance indicators (KPI’s). As we identified in this section, just looking at response time fails to provide a complete picture of how your service is responding, how it will respond, and what investments need to occur to enable it to achieve a high performing status. Included in our review is a look at your payer mix, your collection process, and what are your costs for service.
CPSM’s experts wrote the book on Mobile Integrated Healthcare (MIH). The book is in its second printing and can be found here: “Mobile Integrated Healthcare – Approach to Implementation” published by Jones and Bartlett Publishing.
Our Recent Work with EMS Agencies
Otsego County, New York
Plymouth, Massachusetts
Petaluma, California
Steuben County, New York
National City, California
Franklin County, North Carolina
